Introduction
You have seen a Maxillofacial Surgeon who has recommended surgery to remove a skin lesion (growth). There are many types of skin lesions but the most common types are Basal Cell Carcinoma (BCC) and Squamous Cell Carcinoma (SCC). Both are types of Skin Cancer and need to be removed with an operation to completely cut them out witha clear edge (margin) of normal skin. This leaflet will explain the various ways skin lesions can be removed and some potential complications.
Surgery
This usually takes place with you awake and the area to be operated on made numb by giving injections of Local Anaesthetic. These injections can be painful initially but the area soon goes numb and you should feel no further discomfort until the numbness wears off approximately 1-2 hours after the surgery is completed. There are different types of surgery and the operation you will have will depend on:
a) the size of your skin lesion
b) the location of your skin lesion
c) any vital structures nearby e.g. Eyes, Nose, Lips, Ears.
There are 3 main types of Operation
1. Primary Closure
The wound is closed in astraight line with a row of stitches.
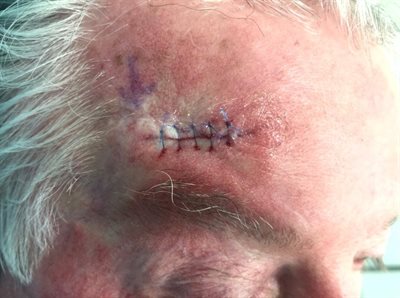
2. Local flap
Removal of skin lesion and closure with a Local Flap
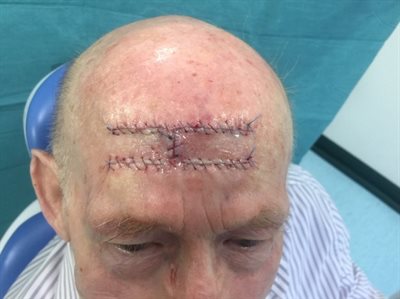
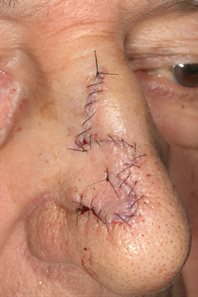
3. Skin graft
Removal of skin lesion and closure with a full thickness skin graft, usually taken fom the neck.
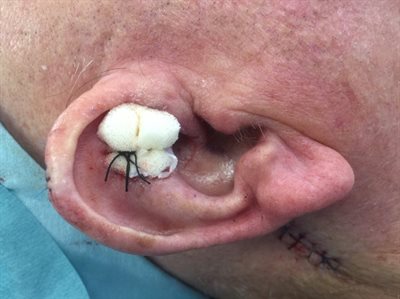
Skin graft used to reconstruct area following removal of lesion.
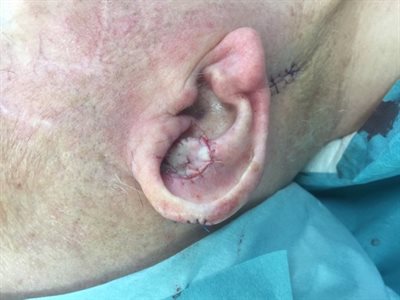
Sponge dressing over skin graft
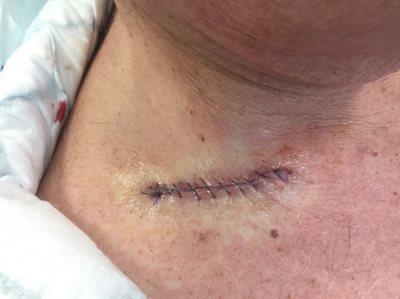
Region where Skin graft was taken from
Post-operative instructions
- You will be given specific instructions for your wound as each operation is unique to the individual.
- The local anaesthetic will start to wear off after 1-3 hours.
- It is normal for the wound to leak spots of blood. Wash your hands with soap and water. Using cooled, boiled water wet the gauze you have been given and squeeze it out. Apply this to the wound and press using medium pressure to the area that is bleeding for 20 minutes. You should be sitting up and relaxed as possible. Avoid lying down as this could make the bleeding worse. The bleeding should stop. If this is not the case, please contact the on- call number below.
- Once the bleeding has stopped, wash your hands again with soap and water; using the flat part of your finger, apply a thin layer of Chloramphenicol eye ointment to cover the stitches.
- Ensure you clean any blood and scabs around the wound with cooled, boiled water twice a day. Apply Chloramphenicol eye ointment morning and evening, to the stiches following this.
- If you have had a skin graft with a sponge dressing stitched in place, please clean the edges around the base of the sponge each day with cooled boiled water and apply a thin layer of Chloramphenicol eye ointment.
- Take pain killers regularly as directed.
- Apply Chloramphenicol eye ointment/ VaselineTM on the day you have your stitches removed.
- It is important to follow these instructions as this will minimise the chances of complications.
NOTE: Chloramphenicoleyeointmentisforyourstitches.Do not put it in your eyes in this case. This is a very small tube, when it runs out, please apply VaselineTM with your own supply.
Early Complications
These include pain, swelling, bleeding, bruising, wound infection and wound break down (where the wound edges fail to heal together).
What to look for
Any redness around the stitches that is getting worse daily.
Increased pain at the wound site, especially a throbbing pain with pus or discharge leaking between the stitches.
The wound will be red for the first 24-36 hours but this should decrease not get worse.
If you are worried you can call the Hospital or your GP for advice.
If you smoke you are more likely to get complications following surgery, if at all possible please do not smoke for 1 week before your operation and 2 weeks after. We understand this can be difficult and would encourage you to seek help from the ‘Help to stop smoking’ team at your GP’s surgery. This may be your opportunity to stop smoking for good!
Follow Up
You will be given an Electronic Discharge Notification (EDN) sheet before you leave the hospital. This will tell you when and where the surgeon has asked for you to be seen to remove your stitches and also when your surgeon would like to see you again in clinic. The surgeon usually asks to see you 6-12 weeks after surgery, however, some people may get a telephone consultation appointment instead of a face to face at the hospital.
Stitches are usually removed by a nurse between 7-14 days after surgery.
All skin lesions are sent to the laboratory for analysis (testing) and your surgeon may write to you with these results before your clinical appointment or telephone consultation.
All operations leave a scar which takes approximately 3 – 6 months to settle. To begin with, your scar will be red and swollen but as the weeks progress, the appearance slowly improves until only a fine line is visible. This could take as long as 12-18 months in some people.
Contact Us
Please Call Maxillofacial Unit 01604 523200 Option 1 – Monday – Thursday 9am-4:30pm, Friday 9am-1pm.
Hospital contact number Out of Hours: 01604 634700, ask the operator to Bleep 4175 and you can speak to the Maxillofacial Doctor who is on-call.
Useful Websites
Other Information
Northampton General Hospital operates a smoke-free policy. This means that smoking is not allowed anywhere on the Trust site, this includes all buildings, grounds and car parks. Leaflets, information, advice and support on giving up smoking and on nicotine replacement therapy are available from the local Stop Smoking helpline on 0845 6013116, the free national helpline on 0300 123 1044, email: smokefree@nhft.nhs.uk and pharmacies.
Car parking at Northampton General Hospital is extremely limited and it is essential to arrive early, allowing ample time for parking. You may find it more convenient to be dropped off and collected.
This information can be provided in other languages and formats upon request including Braille, audio cassette and CD. Please contact (01604) 523442 or the Patient Advice & Liaison Service (PALS) on (01604) 545784, email: ngh-tr.pals@nhs.net.
NGV2308